Oesophagus-Eosinophilic Esophagitis: Did You Know About the Allergic Condition?
M3 India Newsdesk Apr 19, 2024
Explore the enigmatic world of Eosinophilic Esophagitis (EoE), where symptoms, diagnostics, and treatments intertwine in a complex web, challenging medical norms and inviting deeper inquiry.
Case study
- A 40-year-old male presented to our gastroenterology clinic with a complaint of intermittent dysphagia for solids over the past seven months. He described a sensation of food getting stuck in his chest, particularly with meat and bread. He denied any significant weight loss, heartburn, loss of appetite or regurgitation symptoms.
- His medical history was unremarkable for any allergic disorders or autoimmune conditions.
- On examination, the patient appeared well-nourished with no signs of acute distress. There were no palpable masses or lymphadenopathy on neck examination.
- Initial laboratory investigations, including complete blood count and basic metabolic panel, were within normal limits.
- An upper gastrointestinal endoscopy was performed, revealing longitudinal furrows, concentric rings, and, suggestive of oesophagal inflammation. Multiple biopsies were obtained from the oesophagal mucosa, which showed dense eosinophilic infiltration (>15 eosinophils per high-power field) in the absence of reflux changes or evidence of infection.
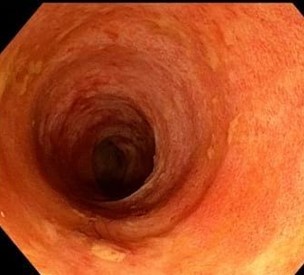
(Click on the image to view)
- Based on the clinical presentation, endoscopic findings, and histological examination, a diagnosis of EoE was made.
- The patient was counselled regarding the chronic nature of the disease and the importance of dietary modifications to avoid known triggers, such as common food allergens (e.g., dairy, wheat, soy).
- He was started on a Proton Pump Inhibitor (PPI) trial to rule out Proton Pump Inhibitor-responsive oesophagal eosinophilia (PPI-REE).
- In addition, he was referred to an allergist for further evaluation of potential food allergies.
- Over the subsequent months, the patient reported significant improvement in dysphagia symptoms with dietary modifications and PPI therapy.
- A repeat endoscopy performed eight months later showed marked improvement in oesophagal inflammation, with a resolution of furrows and exudates.
- Histological examination of the biopsies confirmed a reduction in eosinophilic infiltration (<5 eosinophils per high-power field), consistent with treatment response.
Common clinical presentations include:
- Dysphagia: Dysphagia, or difficulty swallowing, is a hallmark symptom of EoE in adults. Patients may experience a sensation of food sticking in the throat or chest during swallowing, particularly with solid foods.
- Food impaction: Food impaction occurs when ingested food becomes lodged in the oesophagus, leading to acute obstruction. This complication is common in EoE and may require urgent endoscopic intervention for removal.
- Chest pain: Patients with EoE often report chest pain, which is typically centrally located behind the sternum. Unlike typical heartburn associated with gastroesophageal reflux disease (GERD), chest pain in EoE may not respond to antacids.
- Gastroesophageal Reflux Disease (GERD)-like symptoms/refractory heartburn: Some adults with EoE may present with symptoms resembling GERD, such as heartburn and regurgitation. However, these symptoms may be refractory to standard acid-suppressive therapy, raising suspicion for EoE.
- Upper abdominal pain: Upper abdominal pain is another common complaint in adults with EoE. The pain may be diffuse or localised to the epigastric region and can vary in severity.
Clinical manifestations in children
- Feeding dysfunction
- Vomiting
- Abdominal pain
- Dysphagia
- Food impaction
Associations of Eosinophilic Esophagitis (EoE) with other disorders
Food allergies: Common food allergens implicated in EoE include milk, eggs, soy, wheat, and seafood. Elimination diets targeting specific allergens often play a crucial role in the management of EoE.
Environmental allergies: Environmental allergens, such as pollen, mould, and pet dander, have also been implicated in the pathogenesis of EoE. Sensitisation to environmental allergens may contribute to systemic immune activation and mucosal inflammation in the oesophagus.
Asthma: Asthma and EoE frequently coexist, suggesting a shared underlying allergic diathesis. Both conditions involve dysregulated immune responses characterised by eosinophilic infiltration and Th2-mediated inflammation. The presence of asthma may influence the severity and clinical course of EoE and vice versa.
Atopic dermatitis: Atopic dermatitis, a chronic inflammatory skin condition, is commonly observed in patients with EoE. Additionally, skin barrier dysfunction and epithelial barrier defects may play a role in the pathogenesis of EoE.
Diagnostic guidelines for Eosinophilic Esophagitis (EoE)
Recognition of oesophagal dysfunction symptoms:
Patients must exhibit symptoms suggestive of oesophagal dysfunction, including dysphagia, food impaction, chest pain, heartburn, regurgitation, or upper abdominal discomfort. The severity and duration of these symptoms may vary.
Identification of eosinophilic inflammation on oesophagal biopsy:
Histopathological examination of oesophagal tissue specimens is pivotal for confirming EoE diagnosis. Notably, a hallmark feature is the presence of eosinophilic infiltration within the oesophagal mucosa, typically quantified as ≥15 eosinophils per high-power field (HPF). Eosinophils typically disperse diffusely throughout the epithelial layer.
Exclusion of alternative causes:
A thorough evaluation is necessary to rule out other potential contributors to oesophagal symptoms and eosinophilia, such as GERD, infections, eosinophilic gastroenteritis, connective tissue disorders, and medication-induced eosinophil elevation. This may entail additional investigative procedures, including endoscopic biopsy, imaging modalities, laboratory assays, and clinical correlation.
Endoscopic findings in Eosinophilic Esophagitis (EoE)
- Stacked circular rings ("Feline" oesophagus): Circular rings resembling a feline oesophagus are observed in approximately 44% of cases.
- Strictures (Particularly proximal): Strictures, especially proximal strictures, occur in around 21% of patients, contributing to dysphagia and food impaction.
- Attenuation of subepithelial vascular pattern: A diminished subepithelial vascular pattern is noted in approximately 41% of individuals, indicating underlying mucosal inflammation.
- Linear furrows: Linear furrows, resembling oesophagal rings, are present in approximately 48% of cases, reflecting chronic mucosal injury and fibrosis.
- Whitish specks (Eosinophil microabscesses): Whitish specks, indicative of eosinophil microabscesses, are observed in approximately 27% of patients, highlighting local eosinophilic inflammation.
- Small calibre oesophagus: Some patients exhibit a small calibre oesophagus, noted in approximately 9% of cases, which may contribute to dysphagia and impaired bolus transit.
Histological features of Eosinophilic Esophagitis (EoE)
Increased eosinophilic infiltration: The majority of patients exhibit eosinophil counts of at least 15 eosinophils per high-power field (peak value) in at least one biopsy specimen. This eosinophilic infiltration is a hallmark feature of EoE.
Presence of eosinophilic microabscesses: EoE may also be characterised by the formation of eosinophilic microabscesses within the oesophagal epithelium. These microabscesses consist of clusters of eosinophils and are indicative of local inflammation and tissue damage.
Eosinophilic debris and extracellular granules: Histological examination may reveal eosinophilic debris and extracellular granules within the oesophagal epithelium. These findings further support the diagnosis of EoE and suggest ongoing eosinophilic inflammation.
Additional histological findings in Eosinophilic Esophagitis (EoE)
Superficial layering of eosinophils: Eosinophils are predominantly localised within the superficial layers of the oesophagal epithelium, contributing to mucosal injury and dysfunction.
Sheets of eosinophils: Dense aggregates or sheets of eosinophils present within the oesophagal mucosa, suggesting significant mucosal inflammation and tissue damage.
Subepithelial and lamina propria fibrosis and inflammation: Fibrosis and inflammation extend into the subepithelial and lamina propria layers of the oesophagal mucosa, contributing to tissue remodelling and structural changes.
Basal cell hyperplasia: Expansion and hyperplasia of basal epithelial cells within the oesophagal epithelium, indicative of epithelial injury and repair processes.
Papillary lengthening: Elongation of the papillae within the oesophagal mucosa, often observed in response to chronic inflammation and tissue remodelling.
Increased numbers of mast cells, B cells, and IgE-bearing cells: Elevated levels of mast cells, B cells, and IgE-bearing cells within the oesophagal mucosa, reflecting an underlying allergic inflammatory response.
Radiological evaluation in Eosinophilic Esophagitis (EoE)
Barium studies are not typically used as a primary diagnostic tool for EoE due to limited sensitivity, but they can offer valuable insights into anatomic abnormalities and help characterise strictures. Key points regarding radiological evaluation in EoE include:
Anatomical characterisation: Barium studies can identify anatomic abnormalities such as strictures and provide information on the length and diameter of strictures, aiding in treatment planning.
Findings in EoE: Common findings observed in patients with EoE undergoing barium studies include strictures and a ringed oesophagus. These findings complement endoscopic evaluation and provide additional information on luminal narrowing.
Rule out other causes: Barium studies can help rule out alternative causes of symptoms, such as malrotation, which may present with vomiting. This differential diagnosis is essential for accurate management.
Assessment of luminal narrowing: Barium studies are particularly useful for assessing luminal narrowing that may not be evident on endoscopy, especially in children or when combined with the use of a barium-coated pill.
Laboratory investigations: Laboratory tests play a supportive role in the diagnosis and management of EoE.
Serum IgE levels: Elevated serum IgE levels (>114,000 units/L) are observed in approximately 50 to 60% of patients with EoE. This finding underscores the association between EoE and allergic conditions.
Peripheral eosinophilia: Peripheral eosinophilia is seen in 40 to 50% of patients with EoE but is generally mild. In some cases, peripheral blood eosinophil levels may decrease with topical glucocorticoid therapy.
Genetic and molecular markers: Research is ongoing to identify genetic and molecular markers of disease activity in EoE. For example, a 96-gene EoE diagnostic panel has been developed, which may differentiate between active and inactive disease states and identify glucocorticoid exposure.
Evaluation for allergies: Given the strong association between EoE and allergies, evaluation by an allergist is recommended for patients with EoE. Allergy testing can inform dietary therapy and guide the management of concomitant atopic disease.
Other diagnostic tests: Several other diagnostic tests have been evaluated for EoE but are not routinely used. These include functional lumen imaging probe, endoscopic ultrasound, impedance planimetry, mucosal impedance contour analysis, oesophagal manometry, endoscopic confocal laser microscopy, oesophagal string test, and the cytosponge.
Management approaches for Eosinophilic Esophagitis (EoE)
Dietary therapy: Referral to an allergist for food allergy evaluation is recommended for both adults and children. Avoidance of identified allergens (food and environmental) can be effective, following discussion of benefits and drawbacks.
Initial pharmacologic therapy: Proton Pump Inhibitor (PPI) therapy: A trial of PPI therapy for eight weeks is advised. Endoscopy is performed after 8-12 weeks to assess response.
Topical glucocorticoid therapy: Budesonide oral suspension is preferred for its consistent delivery. For adults and pediatric patients (11 years and older), the recommended dose is 2 mg twice daily for 12 weeks. Swallowed fluticasone can be an alternative if budesonide is unavailable.
Management of non-responders to topical glucocorticoids
Options include trying an elimination diet or dupilumab, an alternative treatment.
Maintenance therapy: Consider maintenance therapy with topical glucocorticoids and/or dietary restrictions, particularly in severe cases or those with rapid symptomatic relapse post-initial therapy.
Oesophagal stricture management: Dilation may be necessary for patients with strictures, but it should be approached cautiously due to associated risks. Topical glucocorticoid therapy can alleviate dysphagia and potentially obviate the need for dilation.
Role of acid suppression: Acid suppression may be warranted if reflux is suspected to contribute to symptoms, especially in patients on topical glucocorticoids or dietary therapy.
Long-term monitoring: Patients with stable disease are monitored for recurrent symptoms at least every 12 to 24 months. Endoscopic evaluation is individualised based on symptom changes, need for therapy adjustments, history of oesophagal pathology, and patient preferences.
Disclaimer- The views and opinions expressed in this article are those of the author and do not necessarily reflect the official policy or position of M3 India.
About the author of this article: Dr Jimmy Patel is a practising gastroenterologist in Chennai.
-
Exclusive Write-ups & Webinars by KOLs
-
Daily Quiz by specialty
-
Paid Market Research Surveys
-
Case discussions, News & Journals' summaries