Monkeypox : Another pandemic in making?
M3 India Newsdesk May 31, 2022
Monkeypox is a viral zoonosis with symptoms similar to those seen in the past in smallpox patients. The transmission, clinical manifestations diagnosis and prevention of monkeypox are penned down in this article.
The advent of monkeypox presents a new medical threat to the global community. India has not yet recorded any cases, but states and the national government are closely monitoring the situation.
Understanding monkeypox
Monkeypox is an uncommon illness resulting from infection with the monkeypox virus which is a member of the genus Orthopoxvirus in the family Poxviridae. In addition to the Variola virus (which causes smallpox) and Vaccinia virus (used in smallpox vaccination), the Orthopoxvirus genus also contains the Cowpox virus.
Terminology
The term 'monkeypox' was coined in 1958 after two outbreaks of a pox-like illness occurred in study colonies of monkeys, thus the name 'monkeypox'. The first human case of monkeypox was documented in the Democratic Republic of the Congo (DRC) in 1970, at a time of increased efforts to eradicate smallpox.
Since then, cases of monkeypox have been documented in numerous other central and western African nations. Cases of human monkeypox outside of Africa have been related to foreign travel or imported animals.
Link between monkeypox and smallpox
Clinical manifestations of monkeypox mimic those of smallpox, an Orthopoxvirus disease linked to monkeypox that has been eliminated. Smallpox was more transmissible and often lethal, as around 30 per cent of victims succumbed. The final instance of spontaneously acquired smallpox occurred in 1977, and the disease was proclaimed eliminated globally in 1980 after a global vaccination and containment effort.
All nations have discontinued regular smallpox immunisation using vaccinia-based vaccinations for at least 40 years. Since immunisation also provided protection against monkeypox in the west and central Africa, unvaccinated populations are now more vulnerable to infection with the monkeypox virus.
Although smallpox is no longer a naturally occurring disease, the global health sector remains watchful in case it reappears due to natural causes, a laboratory accident, or purposeful release. To assure worldwide preparation in the event of a smallpox resurgence, researchers are developing new vaccinations, diagnostics, and antiviral drugs.
Transmission
Transmission from animals to humans
- Typically, the virus is transmitted by contact with an infected animal's body secretions or a bite.
- Humans and monkeys are accidental hosts; the reservoir is unknown but presumably rodents. Accidental importation of infected rodents from Western Africa into the United States led to the first human monkeypox illnesses in the Western Hemisphere.
Based on data from an epidemic in the United States in 2003, the route of infection and degree of exposure (e.g., bite wound vs contact with an infected animal) might impact the severity of clinical signs of monkeypox infection.
Transmission from human to human
- Large respiratory droplets may play a role in human-to-human transmission.
- Transmission may also occur by contact with infected skin lesions or lesion debris.
- For droplet transmission, continuous face-to-face contact may be necessary (e.g., within a 6-foot radius for 3 hours in the absence of personal protective equipment [PPE]).
In general, person-to-person transmission is quite low. In May 2022, however, a cluster of cases suggests a significant chance of person-to-person transmission. Sexual contact with infectious skin lesions may be the most probable method of transmission in these clusters. Following more research, additional details will be revealed.
Clinical presentation and symptoms
- The symptoms of monkeypox in people are comparable to but less severe than those of smallpox.
- The first symptoms of monkeypox include fever, headache, muscular pains, and fatigue. The primary distinction between smallpox and monkeypox symptoms is that monkeypox produces lymphadenopathy, while smallpox does not.
- The incubation period (time from infection to onset of symptoms) for monkeypox ranges from 5 to 21 days but is typically 7 to 14 days.
The sickness starts with:
- Fever
- Headache
- Muscle pains
- Backache
- Lymph node enlargement
- Chills
- Exhaustion
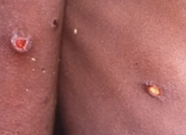
Rashes arise within a few days (sometimes longer) following the patient's fever, and they tend to start on the face before spreading to other regions of the body. As the disease progresses, lesions go through these phases:
- Macules
- Papules
- Vesicles
- Pustules
- Scabs
Typically, the disease lasts two to four weeks. Monkeypox has been linked to the mortality of up to 10% of those who catch it in Africa.
Diagnosis
The clinical characteristics of monkeypox are useful in establishing the diagnosis; nevertheless, laboratory confirmation is required to distinguish this illness from those caused by other possible aetiologies. The following are examples of diagnostic tests:
- Virus isolation (in mammalian cell cultures)
- Electron microscopy
- Real-time polymerase chain reaction (PCR)
- Enzyme-linked immunosorbent assay (ELISA), and
- Immunofluorescent antibody assays
Local and state public health authorities should be alerted if monkeypox is suspected. Varicella, herpes simplex infection, smallpox, and other orthopoxvirus diseases should be considered in the differential diagnosis of a patient with probable monkeypox.
Prevention
To prevent the spread of monkeypox, there are a variety of interventions that may be implemented:
- Stay away from animals that may carry the infection (including animals that are sick or that have been found dead in areas where monkeypox occurs).
- Avoid coming into touch with any things, including bedding, that has been in contact with a sick animal.
- Isolate sick individuals from others who may be susceptible to infection.
- After having contact with sick animals or people, it is necessary to practice proper hand hygiene. For instance, washing your hands with soap and water or using a hand sanitiser containing alcohol.
- When caring for patients, personal protection equipment (PPE) must be worn.
Vaccination
As a result of vaccinia virus immunisation, monkeypox illness may be less severe in those who previously had the smallpox vaccine. A modified vaccinia Ankara (MVA) vaccine (marketed as Imvamune and Jynneos) was authorised in September 2019 for the protection of smallpox and monkeypox.
Several observational studies have shown that smallpox vaccination is around 85 per cent effective in preventing monkeypox. Therefore, previous immunisation against smallpox may result in a lesser disease. Typically, a scar on the upper arm indicates that a person has been vaccinated against smallpox.
The original (first-generation) smallpox vaccinations are not accessible to the general population at this time. Some laboratory or health employees may have gotten a more modern smallpox vaccination to protect them in the case of occupational exposure to orthopoxviruses.
In 2019, a vaccine based on an Ankara strain of modified attenuated vaccinia virus was authorised for the prevention of monkeypox. This vaccination requires two doses, and its availability remains restricted. Due to the cross-protection given by the immune response to orthopoxviruses, smallpox and monkeypox vaccines are formulated with the vaccinia virus.
Postexposure prophylaxis
Certain patients who have been exposed to monkeypox (e.g., direct contact with the patient or items from the patient's room without personal protective equipment) may benefit from postexposure immunisation with the MVA vaccine.
Based on previous evidence on smallpox postexposure vaccination with the vaccinia vaccine, the best period for monkeypox postexposure vaccination is within four days; however, according to the CDC, immunisation may be considered for up to 14 days after a close contact exposure.
Close contact is defined as direct exposure within six feet of a suspected or confirmed case of monkeypox in an animal with respiratory symptoms such as nasal discharge, cough, or conjunctivitis in an environment where the animal has been handled (eg, an exam room).
Vaccinia immune globulin - Since vaccination with the vaccinia virus vaccine is contraindicated in immunocompromised individuals with a history of exposure, the use of vaccinia immune globulin may be suggested.
Infection control precautions - Contact and airborne precautions are required for any broad vesicular rash of unknown cause that includes monkeypox and smallpox in the differential diagnosis.
Persons with suspected monkeypox should be isolated for the first week of the rash until all scabs have peeled and the findings of a throat swab polymerase chain reaction (PCR) are negative.
Patient management
Supportive care
- The majority of people have mild diseases and improve without treatment.
- Hospitalisation for intravenous hydration may be necessary for those who have risk factors for dehydration (e.g. nausea and vomiting, dysphagia).
- The critically sick patient must get supportive care until he or she recovers from the infection.
- Care for monkeypox must be adjusted to ease symptoms, manage complications, and avoid long-term problems.
- Fluids and food should be provided to patients in order to preserve their nutritional state.
- As directed, secondary bacterial infections should be treated.
- The European Medical Association (EMA) approved tecovirimat, an antiviral drug designed for smallpox, for monkeypox in 2022, based on findings from animal and human research. It is not widely accessible yet.
If tecovirimat is utilised for patient treatment, it should preferably be monitored within the framework of clinical research with prospective data collecting.
Mortality
The mortality rate in Central Africa is roughly 10 per cent, and most fatalities occur during the second week of sickness. In contrast, the United States epidemic did not result in any fatalities. This may be due to a healthier patient population, improved availability of supportive medical treatment, and a less virulent type of monkeypox imported from Ghana in West Africa.
Is monkeypox a cause for concern for India?
In India, there are currently no instances of monkeypox. India increased monitoring at all international entry ports for monkeypox infections in response to rising worldwide worries about an unusual epidemic that has led to the suspicion of over 100 cases in areas of Europe, the United States, and Australia. Given that the illness has already spread across continents, India must be very vigilant. In the contemporary age of a shrinking world, viral illnesses propagate rapidly.
- The national government has instructed states and territories to keep a watch on individuals who exhibit signs of monkeypox and have a history of travelling to afflicted nations.
- The Centre further said that questionable samples will be forwarded to the National Institute of Virology in Pune (NIV) for testing.
- The National Center for Disease Control (NCDC) has urged states and Union territories to isolate suspected patients until all lesions have healed and a new layer of skin has grown, or until the treating physician chooses to stop isolation.
Click here to see references
Disclaimer- The views and opinions expressed in this article are those of the author's and do not necessarily reflect the official policy or position of M3 India.
The author is a practising super specialist from New Delhi.
-
Exclusive Write-ups & Webinars by KOLs
-
Daily Quiz by specialty
-
Paid Market Research Surveys
-
Case discussions, News & Journals' summaries