Management of Atopic Dermatitis
M3 India Newsdesk Jun 28, 2024
This article discusses the prevalence, symptoms, and comorbidities of atopic dermatitis (AD), along with current and emerging treatments. It emphasises the importance of skin hydration and individualised therapeutic approaches.
Atopic dermatitis (AD) is the most common form of Eczema which is a commonly used term for skin rash. It is a common and chronically relapsing inflammatory dermatological disorder, prevalent in 5% to 8% of adults and 11% to 20% of children among which approximately one-third of children and half of adults with AD have moderate or severe disease and its course is highly dependent on environmental and genetic factors.
In India, the prevalence of AD is lower compared to Global estimates as per the International Study of Asthma and Allergies in Childhood (ISAAC) but has been reported to be increasing owing to changes in environmental factors. AD has the highest disease burden based on disability-adjusted life-years among dermatological disorders and ranks 15th among all non-fatal diseases.
Symptoms
- AD does not always manifest with the same set of symptoms. Studies have suggested symptoms of AD appear during the initial years of life in around 80% of patients of which there is remission for 60% of the patients in adolescence.
- AD developed during childhood is characterised by eczematous lesions on the flexural areas, nape of the neck, dorsum of the feet and hands.
- Commonly observed lesions in adult patients with AD are lichenified flexural dermatitis alone or associated with head/neck, and hand eczema, and the prurigo nodularis (PN), patients with AD may experience itching, sleep disturbances, poor performance at school/work, and disturbed social, mental, and emotional functioning which might lead to depression and anxiety as reported in a literature search.
- AD is also associated with several other atopic diseases including:
- Asthma
- Allergic rhinitis
- Food allergies
- AD also increases the risk of other non-allergic comorbidities including mental health disorders and other autoimmune- or immune-mediated diseases.
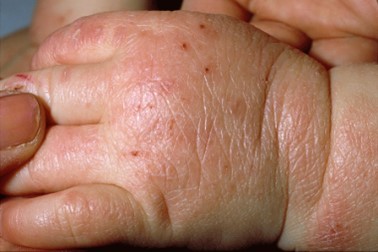
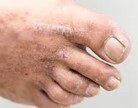
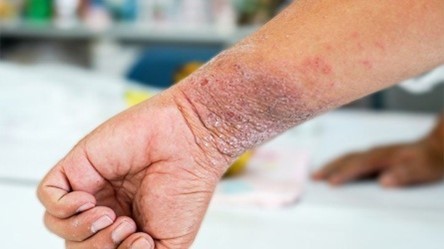
Atopic dermatitis skin lesions
Intervention
- The Barrier Enhancement for Eczema Prevention (BEEP) randomised control trial evaluated the effects of daily emollients during the first year of life on atopic dermatitis and atopic conditions to age 5 years outcome reflects it does not prevent atopic dermatitis, food allergy, and asthma.
- As there has been so much research in the field of gut health, few meta-analyses have suggested probiotic intervention may provide an effective means of preventing AD in children but still, there is not enough data in the literature to respond to questions regarding optimal dosing, optimal time to start treatment and duration necessary to show beneficial effects so has not been implemented in any guidelines.
- Vitamin D levels correlated with AD severity, there has been mixed opinion on the therapeutic outcome of its supplementation and there is further scope of research in our pediatric population.
- Antihistamines or corticosteroids are used during the exacerbation phase. However, while these therapies can mitigate symptoms, their use is often not efficacious enough, and the recurrence rate is still high.
- Evidence-based therapeutic approaches include:
- Promoting skin hydration
- Shunning allergens
- Application of topical therapies including emollients and topical anti-inflammatory medications, concomitantly with most commonly narrow-band UVB (313 nm wavelength) phototherapy and systemic therapies using shared decision-making between patients and clinicians should be considered.
- However, there is difficulty in adherence to phototherapy as it has to be delivered at medical centres usually 2-3 times a week for a few months which hampers the patient or caregiver's work schedule.
Treatment
- Regular use of emollients and moisturisers is the cornerstone of nonprescription treatment for both adult and juvenile AD.
- Guidelines currently recommend liberal and frequent reapplication of moisturisers throughout the day and soon after bath to avoid drying and retain moisture of the skin.
- During an AD flare, wet-wrap therapy (WWT) is a process that involves the application of moisturiser or Topical Corticosteroid (TCS ) to the involved skin followed by a wrap of a damp bandage or gauges to rehydrate the skin which is left on for 8–24 hours.
- For individuals with AD in addition to baseline therapy like emollients and bathing practices topical calcineurin inhibitor (pimecrolimus, tacrolimus), moderate-potency topical corticosteroid, Crisaborole which is a phosphodiesterase 4 (PDE-4) inhibitor may be used for topical treatment of mild to moderate AD in children 3 months of age and older and Ruxolitinib cream are among the most effective in improving AD outcomes in milder disease.
- Topical calcineurin inhibitors (TCIs) are used in the treatment of pediatric AD, often as adjuncts to topical corticosteroids (TCS) in lower potency.
- For the moderate to severe form of AD systemic therapies include biologics like dupilumab which through inhibition of the IL-4 and IL-13 signaling cascade reduces the Th2 inflammatory response which is the key to the pathophysiology of AD.
- Tralokinumab is another IL-13 inhibitor which is already approved for use in adult patients. The other systemic therapies used currently are Janus kinase inhibitors, also known as JAK inhibitors like Upadicitinib and Abrocitinib are currently FDA-approved for the treatment of AD as published in the latest guideline of the Journal of American Academy of Dermatology (JAAD).
- Upadacitinib was recently approved in 2022 for pediatric patients 12 years of age and older with refractory moderate to severe AD.
- Other systemic therapies include methotrexate, azathioprine, cyclosporine, mycophenolate mofetil and systemic steroids despite being cost-effective options are used with conditional recommendations due to their long-term adverse effects, the need for stringent laboratory monitoring and availability of better systemic therapies as discussed above and we also stress upon the need of cost-effectiveness analyses comparing older to newer treatments in our population.
- Hadley et al have also mentioned the benefits of bleach baths, Alpine Climate Treatment, and stress-relieving techniques in patients of AD and since the list of potential treatments for this disease is long and not limited to those described above which includes the standard pharmaceutical agents, nonprescription adjuvants, and alternative therapies.
- As our understanding of the pathophysiology of Atopic dermatitis continues to grow, the treatment options will increase over the coming years. Clinicians should ideally aim to strike a balance between symptom control and minimal associated adverse effects individualising the limitation of cost constraints.
Disclaimer- The views and opinions expressed in this article are those of the author and do not necessarily reflect the official policy or position of M3 India.
About the author: Dr Manish Khanna is MBBS, DNB, MNAMS working as a physician at Uttar Pradesh Provincial Medical Services (UPPMS), Lucknow.
-
Exclusive Write-ups & Webinars by KOLs
-
Daily Quiz by specialty
-
Paid Market Research Surveys
-
Case discussions, News & Journals' summaries