Gastric Volvulus: Practice Essentials And Clinical Management
M3 India Newsdesk Apr 26, 2024
This article delves into the complexities of gastric volvulus, from its diagnosis to management, providing valuable insights for healthcare professionals to enhance patient care and outcomes.
Gastric volvulus is a rare but potentially life-threatening condition characterised by the abnormal rotation of the stomach. Diagnosis is often challenging due to its nonspecific clinical presentation and rarity.
We present a case of gastric volvulus diagnosed incidentally during upper gastrointestinal endoscopy, highlighting the importance of considering this condition in the differential diagnosis of upper gastrointestinal symptoms.
Case presentation
- A 65-year-old male presented to the gastroenterology clinic with complaints of recurrent episodes of epigastric discomfort, bloating, and postprandial vomiting over the past month.
- His medical history was notable for gastroesophageal reflux disease (GERD) and hiatal hernia, for which he was on proton pump inhibitor therapy.
- Physical examination revealed mild tenderness in the epigastric region, but no signs of peritoneal irritation were present.
Investigations
- Given his symptoms and medical history, an upper gastrointestinal endoscopy was performed to evaluate the cause of his symptoms and assess the status of his hiatal hernia.
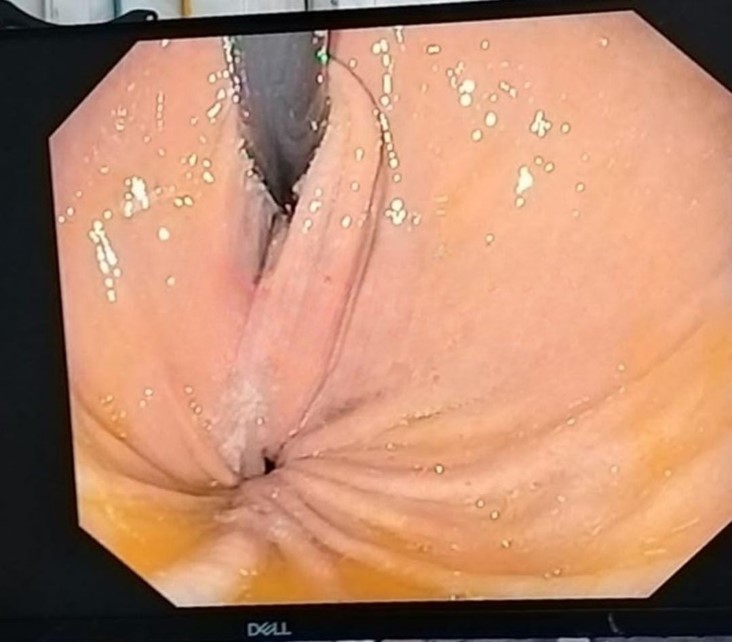
- During endoscopy, a striking finding of an intrathoracic gastric fundus was observed, suggestive of gastric volvulus. The endoscope could not be advanced further due to the torsion of the stomach, confirming the diagnosis.
Management and follow-up
- Following the endoscopic diagnosis of gastric volvulus, the patient was referred for urgent surgical evaluation.
- Contrast-enhanced computed tomography (CT) of the abdomen and chest was performed to further characterise the extent of gastric rotation and assess for associated complications such as gastric ischemia or perforation.
- Surgical intervention was deemed necessary, and the patient underwent laparoscopic gastropexy to secure the stomach and prevent recurrent volvulus.
Outcome
- The patient had an uneventful postoperative course and experienced the resolution of his symptoms.
- Follow-up endoscopy performed six weeks postoperatively demonstrated proper positioning of the stomach, with no evidence of volvulus or obstruction.
- The patient remained symptom-free at subsequent follow-up visits, highlighting the successful management of gastric volvulus in this case.
Introduction
- Gastric volvulus occurs when the stomach rotates along its long or short axis, resulting in diverse levels of gastric outlet obstruction. This condition can manifest abruptly or gradually over time.
- When the stomach rotates beyond 180°, it triggers complete gastric outlet obstruction, raising the spectrum of ischemia or strangulation, and potentially culminating in necrosis, perforation, and abdominal sepsis.
- Acute gastric volvulus carries a substantial risk of mortality if overlooked, emphasising the critical importance of swift diagnosis and intervention.
Risk factors associated with gastric volvulus include
- Age over 50 years
- Diaphragmatic abnormalities such as para oesophagal hernia, hiatal hernia, or other diaphragmatic hernias
- Diaphragmatic eventration
- Phrenic nerve paralysis
- Other anatomical gastrointestinal abnormalities, including abnormalities of the stomach or spleen
- Kyphoscoliosis
Pathogenesis
- The pathogenesis of gastric volvulus involves the abnormal rotation of the stomach along either its horizontal or vertical axis.
- Normally, the stomach's position is stabilised by several ligaments, including the gastrocolic, gastrohepatic, gastrosplenic, and gastrophrenic ligaments, which secure it to surrounding abdominal structures and the diaphragm. These ligaments, in conjunction with the gastroesophageal junction and pylorus, help maintain the stomach's position and prevent rotation.
- The degree of gastric outlet obstruction experienced correlates with the extent of rotation when the rotation exceeds 180°, complete gastric outlet obstruction ensues, whereas lesser degrees of rotation results in partial obstruction.
- Chronic rotation of the stomach can have further consequences. It can impede venous return and elevate capillary pressure, potentially leading to gastric bleeding due to compromised circulation.
Classification of gastric volvulus
Primary versus secondary gastric volvulus
- Primary (Idiopathic) gastric volvulus: Occurs due to abnormalities in the gastric ligaments, such as agenesis, elongation, or disruption. Commonly presents with chronic symptoms and can result from conditions like kyphoscoliosis.
- Secondary gastric volvulus: Arises from other anatomical abnormalities, including para oesophagal hernia, diaphragmatic hernia (Morgagni hernia, Bochdalek hernia), diaphragmatic eventration, or phrenic nerve paralysis. Often associated with acute symptoms and occurs in two-thirds of gastric volvulus cases.
Organ axial versus mesenteroaxial volvulus
- Organ axial rotation: Involves rotation along the stomach's long axis, where the greater curvature comes to rest superior to the lesser curvature. Commonly associated with secondary etiologies and poses a higher risk of strangulation.
- Mesenteroaxial rotation: Involves rotation around the stomach's short axis, with the antrum displaced above the gastroesophageal junction. Typically partial (<180°) and not commonly associated with secondary defects.
Acute versus chronic gastric volvulus
- Acute gastric volvulus: Results from rotation >180°, leading to acute gastric outlet obstruction. Often presents with sudden-onset symptoms.
- Chronic gastric volvulus: Manifests with intermittent or chronic symptoms, typically associated with partial gastric obstruction. Acute symptoms may superimpose on the chronic condition.
Clinical presentation of gastric volvulus
1. Acute gastric volvulus
Symptoms
- Patients typically present with acute abdominal or lower chest pain accompanied by severe vomiting, which may become unproductive.
- Borchardt's triad, consisting of pain, vomiting, and inability to pass a nasogastric tube, is present in up to 70% of cases.
- Hematemesis may occur due to mucosal ischemia or tears from vomiting.
- Additional symptoms may include pain related to pancreatic or omental ischemia, omental avulsion, or splenic rupture.
Physical examination
- Abdominal distention with dullness to percussion due to dilated, fluid-filled stomach.
- Signs of volume depletion may be evident, along with gastric sounds auscultated in the chest.
- Signs of peritonitis (rigidity, rebound tenderness) may indicate significant gastric ischemia or perforation.
- The acute presentation can mimic acute coronary syndrome, leading to diagnostic challenges.
2. Chronic gastric volvulus:
Symptoms
Patients may experience mild upper abdominal discomfort, distension, bloating, retching, non-bilious vomiting, dysphagia, early satiety, heartburn, or symptoms suggestive of pancreatitis.
Laboratory findings
Chronic anaemia from gastric ulceration due to abnormal stomach rotation may be evident. Elevated pancreatic enzymes may also be observed.
Diagnostic evaluation of gastric volvulus
Acute Symptoms
- Plain radiography: Initial diagnostic test for suspected acute gastric volvulus. Classic findings include a single large, spherical gas bubble in the upper abdomen or chest with an air-fluid level. Organoaxial volvulus presents with a horizontal stomach position, while mesenteroaxial volvulus exhibits two air-fluid levels on upright films.
- Computed tomography (CT): Preferred if classic features are absent on plain radiography but suspicion for acute gastric volvulus remains. CT demonstrates abnormal stomach positioning, and relationship to surrounding structures, and identifies associated anatomical abnormalities.
- Findings on CT: Dilated stomach, abnormal position (often in the chest), and swirl sign indicative of rotation. Signs of gastric necrosis include pneumatosis of the gastric wall, free air/fluid outside the gastric wall, and lack of contrast enhancement of the gastric wall.
Chronic symptoms
- Plain Radiography and CT: Utilised to demonstrate abnormal stomach positioning in patients with chronic symptoms. Findings may be subtle, with less dramatic stomach bubbles and the presence of air in the distal bowel in cases of incomplete volvulus.
- Upper gastrointestinal (UGI) series: Sensitive and specific when performed with the stomach in the "twisted" state, showing an inverted greater curve above the lesser curve (organoaxial volvulus) or pylorus above gastric fundus (mesenteroaxial volvulus). Limited in identifying other anatomical abnormalities associated with secondary volvulus.
- Upper endoscopy: Although low sensitivity for diagnosing gastric volvulus, helpful for ruling out other upper gastrointestinal diseases and aiding in nasogastric tube placement or stomach fixation using a percutaneous gastrostomy (PEG) tube.
Differential diagnosis of gastric volvulus
1. Other Causes of acute gastric distention and outlet obstruction:
Conditions such as gastric outlet obstruction from peptic ulcer disease, tumours (benign or malignant), strictures, or inflammation may present with acute abdominal pain and gastric distention on imaging studies.
Psychological disorders can also lead to acute gastric dilation in the absence of mechanical obstruction. However, the stomach contour typically maintains a normal shape rather than assuming a spherical contour seen in gastric volvulus.
2. Gastric outlet obstruction aetiologies
A thorough assessment of past medical history may reveal clues suggesting alternative causes for nausea, vomiting, and abdominal pain. Pathologies causing gastric outlet obstruction, such as masses or inflammation, may be evident in imaging studies.
3. Differential diagnosis of abdominal pain
Various causes of abdominal pain beyond gastric volvulus should be considered, including gastrointestinal, hepatobiliary, pancreatic, and gynaecological etiologies. These encompass conditions such as appendicitis, cholecystitis, pancreatitis, and ovarian torsion.
4. Gastroparesis and other gastric motility disorders
Gastroparesis, characterised by delayed gastric emptying without mechanical obstruction, can present with symptoms overlapping with gastric volvulus, such as nausea, vomiting, and abdominal pain. Other gastric motility disorders should also be considered in the differential diagnosis.
Initial treatment of gastric volvulus
Patient stabilissation
- Administer fluid resuscitation and correct electrolyte abnormalities promptly.
- Initiate broad-spectrum antibiotics early for suspected gastric ischemia, perforation, or mediastinitis.
Gastric decompression
- Nasogastric tube decompression: Immediately place a nasogastric tube by a knowledgeable healthcare provider for patients with acute symptoms and severe gastric distention on imaging suggestive of gastric volvulus.
- Endoscopic-assisted decompression: Endoscopy can aid in nasogastric tube placement if bedside attempts fail. Endoscopic decompression can be performed under vision, with minimal insufflation, followed by nasogastric tube placement.
Subsequent care
- Confirm the position and effectiveness of the nasogastric tube through repeat abdominal imaging. Maintain the nasogastric tube to decompress the stomach until definitive repair.
- Monitor for resolution of symptoms, stability, and signs of gastric necrosis or abdominal sepsis. Definitive treatment should occur during the index hospitalisation once the patient is stabilised.
- Immediate surgery is warranted in cases of unsuccessful gastric decompression, confirmed gastric perforation or mediastinal contamination, refractory shock, or severe sepsis.
Endoscopic evaluation
Stable patients with persistent or recurrent symptoms or mild sepsis may benefit from endoscopic evaluation. Endoscopic evidence of gastric ischemia or necrosis mandates immediate surgery, while the absence of ischemia may allow for delayed surgical repair.
Definitive treatment of gastric volvulus
Immediate surgery
- For unstable patients, immediate open surgery is recommended. Reduction and derotation of the stomach should be performed, with careful examination for areas of ischemia.
- Partial or subtotal gastrectomy may be necessary for necrotic tissue. Repair of anatomic defects, such as paraesophageal hernia, is essential to prevent recurrence.
- Damage control laparotomy may be considered for patients with metabolic derangements, followed by a planned second look for definitive repair.
Delayed definitive treatment
- Clinically stable patients with acute or chronic gastric volvulus who respond to resuscitation and decompression may undergo planned definitive treatment after diagnostic evaluation.
- Goals include restoring the stomach to a normal position, repairing anatomic defects, and preventing future rotation.
Primary gastric volvulus
- For primary chronic gastric volvulus, gastric fixation following successful derotation may be sufficient.
- Surgical gastropexy or endoscopic gastropexy using percutaneous endoscopic gastrostomy (PEG) tubes can be performed based on patient condition and preference.
Secondary gastric volvulus
- Symptomatic patients with secondary gastric volvulus should undergo surgical repair of the associated anatomic defect, such as paraesophageal hernia repair.
- Repair involves reduction and derotation of the stomach, removal of necrotic tissue, and closure of the defect.
- Gastric fixation may not be required if anatomic defects are adequately repaired.
Minimally invasive surgery
Minimally invasive laparoscopic or robotic repair is feasible and offers advantages such as reduced morbidity and shorter hospital stays, especially for older adult patients with medical comorbidities.
Poor surgical candidates
- Endoscopic derotation and gastric fixation with PEG tubes are options for patients who are poor surgical candidates.
- PEG tubes provide gastric fixation and are left in place for adhesion formation between the stomach and abdominal wall.
- Loosening of fixation bars is necessary to prevent erosion and leakage. Most patients should eventually undergo definitive surgical management if possible.
Recurrence
- Recurrence of gastric volvulus, especially if left unrepaired, is relatively common, with reported rates of recurrent symptoms in a significant proportion of conservatively managed patients. However, there is limited data on recurrence following surgical repair.
- Studies comparing different surgical approaches have shown varying recurrence rates, with laparoscopic approaches potentially associated with higher recurrence rates compared to open surgery.
- Recurrence rates associated with paraesophageal hernia repair often performed concomitantly with gastric volvulus repair, have been reported separately.
- Despite the risk of recurrence, surgical repair has been shown to significantly improve the quality of life for patients, with studies demonstrating improvements in social function and physical quality-of-life scores. Overall, the risk for general symptom recurrence after surgical repair appears to be low, highlighting the effectiveness of definitive treatment in managing gastric volvulus.
Disclaimer- The views and opinions expressed in this article are those of the author and do not necessarily reflect the official policy or position of M3 India.
About the author of this article: Dr Jimmy Patel is a practising gastroenterologist in Chennai.
-
Exclusive Write-ups & Webinars by KOLs
-
Daily Quiz by specialty
-
Paid Market Research Surveys
-
Case discussions, News & Journals' summaries