Malaria, scrub typhus, and typhoid in children: How to approach?: Dr. Balaji C & Dr. Janani A
M3 India Newsdesk Jul 07, 2020
Dr. Balaji Chinnasami and Dr. Janani Arul, in this article discuss 3 cases- malaria, scrub typhus, and typhoid presenting in children. They provide assistance to general practitioners on how to approach each case and provide readymade, evidence-based prescriptions.

Malaria
A 5-year-old boy weighing 17 kg presents with fever for 5 days. He has high-grade continuous fever, relieved by medication alone. Throat was normal and other system examination was normal. There was decreased oral intake with two episodes of vomiting.
Science behind management
- Classic periodicity, shivering, and sweating is not seen in young children. It can mimic any febrile illness.
- Splenomegaly may take many days to develop.
- Demonstration of malarial parasite establishes diagnosis but only 50% have positive smears.
- Antigen-based rapid diagnostic tests (RDT) gives quick results and will be handy in office practice. Caution is advised about false positive results.
Investigations to run
- Complete haemogram - Anaemia is often present
- Peripheral smear for malarial parasite
- Rapid diagnostic tests for malaria
Rx
- Vivax malaria- Chloroquine for 3 days and primaquine for 14 days to kill extra-erythrocytic forms of parasite
- Falciparum malaria- Artemisinin combination therapy for 3 days and single gametocidal dose of primaquine

Advice to give to parents
- Give extra fluids like tender coconut water, lassi, buttermilk, and sips of water to address dehydration.
- Report to casualty immediately if danger signs like convulsions, lethargy or unconsciousnesss, inability to drink fluids, constant vomiting, inability to pass urine for six hours, respiratory distress, or severe pallor presents.
Scrub Typhus
A 10-year-old child presented with history of fever and myalgia for 5 days and headache and vomiting for 3 days. On examination, the child had a temperature of 102.4ºF. Vital signs were stable and sensorium was normal. On local examination the child also had maculopapular rashes involving the palms and soles and eschar on the left axilla. Systemic examination revealed significant cervical lymphadenopathy (1.5 cm x 1.5 cm) and hepatomegaly (liver span was 8 cm).
Science behind management
- Scrub typhus is a rickettsial infection caused by Orientia tsutsugamushi.
- It is transmitted via the bite of larval stage mite (Chigger).
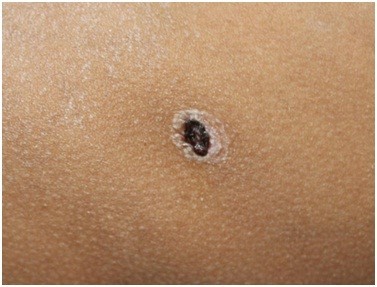
- A single painless eschar with an erythematous rim at the site of the chigger bite is seen in 7 to 65% of cases.
- Eschar is commonly identified in axillary, groin region and behind the ear lobes.
Investigations to run
Haemoglobin of 10.8 g/ dL, total leukocyte count of 4400/mm3, with normal differential count, platelet count of 73,000/mm3.
Lab Diagnosis
Laboratory parameters that are suggestive of rickettsial infection are:
- Leukopenia with a shift to left in early stages and leukocytosis later on
- Thrombocytopenia
- Raised ESR and CRP
- Hypoalbuminaemia
- Elevated hepatic transaminases
The confirmatory test- serological test (Scrub IgM ELISA) which has high sensitivity and specificity.
Rx
| Drugs | Dose | Duration |
|
Tablet Doxycycline 100 mg (1st line) |
1 -0- 1 (4 mg/kg/day) Maximum dose: 200 mg/day |
5 days |
|
Tablet Azithromycin 250 mg (Alternative 2nd line) |
1 -0 -0 10 mg/kg/day |
5 days |
| Tablet Paracetamol 500 mg |
1-1-1 (15 mg/kg/dose) |
SOS |
| Tablet Pantoprazole 40 mg | 0-1 | 5 days |
Advice to give to parents
- Preventing vector bite is the most effective strategy; avoid exposure to vector infested habitats
- Hot water washing and hot drying effectively kills ticks on cloths
- Pets in the hoursehold should be protected with medications or tick collars and periodic de-ticking should be done
Typhoid Fever
A 6-year-old child weighing 15 kg presented with a history of fever for 4 days and vomiting and loose stools for 3 days. On examination, the child had a temperature of 101.4ºF. Other vital signs were stable and sensorium was normal. Systemic examination revealed splenomegaly
Science behind management
- Enteric fever is caused by Salmonella typhi, and less-severe disease is caused by Salmonella paratyphi (A, B or C).
- The bacteria is transmitted by faecal-oral transmission (contaminated food, water and poor sanitation).
- Fever with gastrointestinal symptoms, hepatomegaly and soft splenomegaly are the usual presenting symptoms. The child is usually toxic looking.
- Due to the emergence of multidrug resistant strains, fluoroquinolones and third generation cephalosporin are the drugs of choice.
- Proper sanitation and hygiene practices are the cornerstone of prevention.
- It is a vaccine-preventable disease, 2 vaccines are available (Vi-PS conjugate and Vi-PS polysaccharide).
Investigations to run
- Haemoglobin of 11 g/ dL, total leukocyte count of 22000/mm3, with neutrophilic predominance, platelet count of 92,000/mm3
- USG abdomen to check cholecystitis with minimal ascites and splenomegaly
- Nonspecific parameters- mild anaemia, leukopenia or leukocytosis, thrombocytopenia and elevated hepatic transaminases
Confirmatory tests
- 1st week: Positive blood culture (S. typhi or S. parathyphi) along with culture sensitivity
- 2nd week: Positive Widal test (Salmonella typhi O or H titre >1:160 or Salmonella paratyphi AH or BH >1:160).
- Ultrasonography- Hepatomegaly, splenomegaly, gall bladder involvement
Rx
| Drugs | Dosage | Duration |
| Uncomplicated typhoid | ||
|
Tablet Cefixime 200 mg (1st line) |
1 – 0 - 1/2 (15-20 mgkg/day) |
7-14 days |
|
Tablet Azithromycin 250 mg (alternative) |
3/4 - 0 - 0 (10 mg/kg/day) |
7 days |
| Syrup Paracetamol 250 mg | 5 ml | SOS |
| Severe typhoid | ||
| Injection Ceftriaxone |
500 mg- 0 to 500 mg (75 mg/kg/day) |
10-14 days |
Advice to give to parents
- Ensure proper sanitation measures. Advice parents regarding proper storage of drinking water and milk at home.
- Vaccination
| Vaccine | Dosage | Booster |
| Vi-PS conjugate (conjugate typhoid) - Preferred one | 1 dose at 6-12 months | Not recommended at present |
| Vi-PS (polysaccharide) | Single dose at 2 years of age | Revaccination every 3 years |
Disclaimer- The views and opinions expressed in this article are those of the author's and do not necessarily reflect the official policy or position of M3 India.
Dr. Balaji Chinnasami is a Professor of Paediatrics and Medicine at a reputed medical college in Chennai.
Dr. Janani Arul is an Assistant Professor of Paediatrics from Chennai.
-
Exclusive Write-ups & Webinars by KOLs
-
Daily Quiz by specialty
-
Paid Market Research Surveys
-
Case discussions, News & Journals' summaries